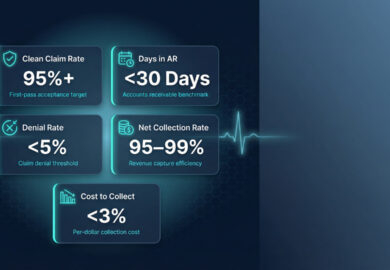
Measuring Medical Billing Performance
Healthcare practices need to follow a few basic activities like managing denials, scrubbing or resubmitting claims, increasing collections, etc. to ensure reimbursement for the care provided to the patient. But to ensure that healthcare practices remain profitable, the healthcare practice needs to track key billing metrics. These KPIs are vital for understanding the financial performance of the healthcare practice, and accordingly for following best industry practices for protecting cash flow.

Some of the Billing KPIs that your Healthcare practice needs to tracks are:
Clean Claims Ratio – A clean claim is the claim that is paid at first submission. A clean claim is never rejected, is not a preventable denial , never been filed more than once and contains no errors. A clean claim improves the speed and amount of reimbursement, and also improves patient satisfaction. A Clean Claims ratio is the percent of clean claims in all the submitted claims. Since Cclean claims are reimbursed faster so the healthcare practice need to evaluate the time spent reworking denied claims and pinpoint the reasons.
Generally, the practices have a clean claims ratio of 70%-85%, but having a clean claims ratio of more than 90% or 95% is also indicative of a successful Billing strategy.
Denial Rate – Denial rate is in a sense opposite of clean claims rate. Denial rate is calculated by dividing number of denied claims by number of billed claims. Some practices also working by dividing monetary amount denied by the amount billed. The practices should strive for a low claims denial rate. Denial Rate between 5% and 10% is the industry average.
In our experience, the high denial rates are caused by:
- Missing information. When a required field is incorrectly filled or the information is missed on the claim form, then it causes a claim denial.
- Duplicate claim or service. When multiple claims for same service are inadvertently submitted with the same provider information.
- The payer doesn’t cover service. Most health insurances have a set of procedures to be covered under the health plan, knowing that list of procedures comes under the purview of the healthcare practices. So before administering services, it is essential to know what will be covered and what will not be covered.
- Improper or lack of coding. This is the most common type of mistake made by the healthcare practices. So it is really important to have the claim submitted to the fullest level of specificity with all the modifiers or identifiers properly included.
- The patient is ineligible for services. Having a VOB at the very onset of the visit is an important way to make sure that the patient is eligible for the services or is ready to pay the dividend, if required.
- The claim is missing authorizations. It is really important to have the utilization review for the care completed at all the required times. Without proper authorization, the claim has a higher chance of getting denied.
- The time limit for filing has expired. It is required to set your processes according to the guidelines of the healthcare payers and have the correct claims submitted in that specific window.
Days in Account Receivable – Days in A/R represents the average length of time it takes for a claim to be paid. Delayed cashflow leads to lost investment opportunities. While industry benchmark for A/R is 30 days, healthcare practices need to maintain atleast 45 days for A/R with anything above 60 days raising a red flag for them.
The first step to calculating A/R is choosing the length of time for which it needs to be calculated. Then the following steps should be performed:
- Adding posted charges for your chosen time period
- Subtracting credits received
- Dividing by the number of days in that period
- Finally, divide your total accounts receivable by the average daily charges.
Closely related to days in A/R is the 0-60 percentage. This KPI represents the percentage of insurance A/R aging in the two youngest buckets: 0-30 days and 31-60 days. Payments due are sorted into the bucket that represents how many days ago the service was billed. To calculate the 0-60 percentage, divide the combined A/R in the 0-30 bucket and the 31-60 bucket by your total A/R.
Net Collection Ratio – This is ultimate indicator of collection success and billing efficiency. Net collections ratio is the percentage of total reimbursements collected out of the total allowed amount. Net collections gives you a realistic picture on what is expected to be received in terms of reimbursements. It reflects how denial rates, unreimbursed visits, and other factors affect revenue.
If your NCR is lower than 90-100% after write-offs, you should consider an audit of billing practices.
Elixir comes in with its powerful billing system, which is specially designed for healthcare practices. The intuitive and automated systems increase the accuracy of your claims and powerful reporting capabilities make business intelligence much easier.
Elixir Practice Management Suite is a comprehensive solution consisting of four modules that fit rightly into your healthcare business irrespective of your facility size and type. The Elixir Contact Center module helps manage the entire facility census and the patient intake process. At the same time, the Elixir EHR solution aims at delivering an end-to-end seamless patient care experience. The third module is Elixir Billing, and it effectively fetches data from any EHR platform to process medical claims and manages the entire revenue cycle. Elixir Patient Portal is the last module, and it provides an integrated experience for the patients.
Do fill out this contact form if you feel that Elixir will be an asset to your system.
Recent Posts
5 EHR Metrics to Improve Revenue Cycle & Healthcare IT
Categories
Recent Comments
Archives
- May 2026
- April 2026
- March 2026
- December 2025
- November 2025
- September 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- November 2024
- September 2024
- July 2024
- April 2024
- February 2024
- November 2023
- September 2023
- August 2023
- May 2023
- February 2023
- January 2023
- July 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- March 2021
- October 2020
- May 2020