Voice Recognition for Clinical Notes: What Actually Works in Modern EHRs
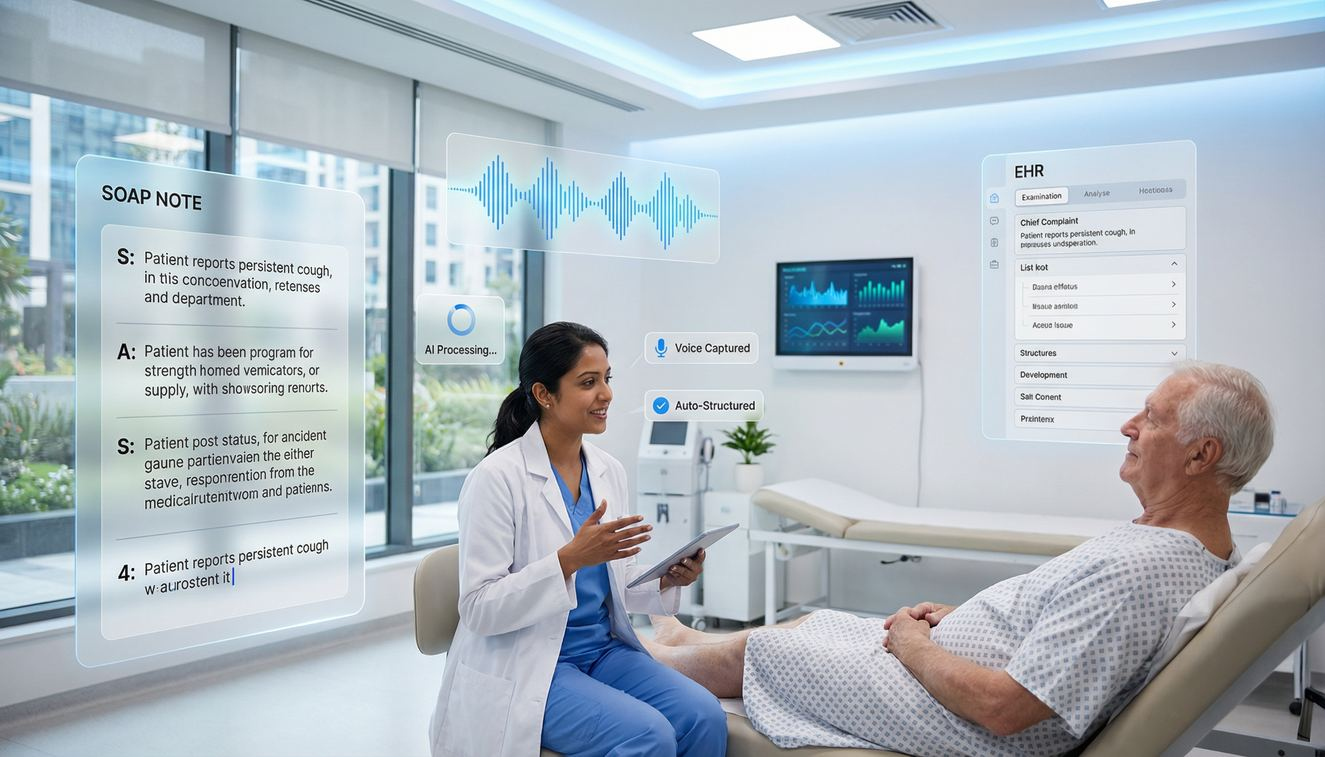
Introduction
There was a time when “voice recognition in healthcare” simply meant dictating into a microphone and hoping the system got your words right. Anyone who used those early tools remembers the frustration misheard terms, constant corrections, and workflows that felt slower than typing.
Fast forward to today, and the landscape has changed dramatically.
Voice recognition in healthcare has evolved across three clear stages:
- Dictation → “Say it, get text”
- Transcription → “Capture conversations”
- Ambient + AI Structuring → “Generate clinical notes automatically”
- Only the third stage actually moves the needle.
Voice is no longer just an input method. It’s becoming the primary interface for clinical documentation. But not everything you hear in the market actually works in real clinical settings. The gap between demos and day-to-day usability is still very real.
So let’s cut through the noise and talk about what genuinely works today in EHRs when it comes to voice recognition for clinical notes.
Here is something no vendor brochure will say plainly: most healthcare organizations in 2026 are still one phishing email away from a serious breach. The tools have improved. The attackers have improved faster.
Electronic Health Records hold a patient’s most sensitive information — diagnoses, medications, mental health notes, financial data. Protecting that data is not just a legal requirement. It is a fundamental duty to the people who trust you with it.
This guide cuts through the noise. We will cover the real threats, where EHR security breaks down, what HIPAA demands in 2026, and the practical steps you can take starting this quarter.
A patient’s medical record is worth up to 40 times more than a stolen credit card on the dark web. Cybercriminals know this. Does your security posture reflect it?
From Dictation to Ambient Intelligence
The biggest shift has been from active dictation to passive listening.
Instead of the clinician stopping to dictate, modern systems can sit quietly in the background, listening to the entire conversation between doctor and patient. This is what’s commonly referred to as ambient listening or an AI scribe.
But the real value is not in listening. It’s in understanding.
Modern systems:
- Identify speakers (provider vs patient)
- Extract clinical context (symptoms, history, plan)
- Generate structured drafts automatically
- In a physical consultation, a device captures the interaction without interrupting the flow. In virtual visits, the system integrates directly into the call. Either way, the goal is the same: let the clinician focus on the patient, not the screen.
What makes this powerful isn’t just transcription. It’s what happens after.
The system identifies who said what, extracts medically relevant details, and turns a free-flowing conversation into something structured history, symptoms, assessment, and plan. By the end of the visit, you’re not staring at a blank note. You’re reviewing a near-complete draft.
That shift from creating documentation to reviewing it is where the real value lies.
Transcription Alone Isn’t Enough
One of the biggest misconceptions is that good transcription equals good documentation. It doesn’t. What actually works is intelligent structuring.
A raw transcript, even if perfectly accurate, is still just a wall of text. Clinicians don’t document in paragraphs they document in structured formats. SOAP notes, specialty templates, problem-oriented records these require organization, not just accuracy.
What works today are systems that bridge this gap.
They don’t just transcribe; they interpret and map. A conversation about symptoms becomes HPI. A discussion about next steps becomes the plan. Medications, diagnoses, and observations get slotted into the right sections automatically.
Even better systems offer flexibility. After a visit, clinicians can see:
- the full transcript,
- an AI-generated summary,
- and a structured note draft.
From there, they can decide what to keep. Some prefer verbatim documentation for legal clarity. Others prefer concise summaries. The best workflows support both, without forcing a rigid approach.
Dictation Isn’t Dead It’s Evolved
With all the excitement around ambient AI, it’s tempting to assume dictation is obsolete. It’s not.
In fact, dictation is still one of the most reliable and preferred methods in many scenarios. The difference is that it’s no longer standalone it’s enhanced.
Modern EHRs allow clinicians to dictate directly into specific fields. Instead of recording a long monologue, you can dictate just the assessment or update the plan. The transcription appears instantly, and you can pause, replay, or edit as needed.
But what really changes the game is what happens after dictation.
Now, you can take a long dictated input and ask the system to:
- clean it up into clinical language,
- summarize it,
- or convert it into a structured format.
This transforms dictation from a raw input tool into a smart clinical assistant.
In practice, clinicians often use a mix: ambient listening captures the bulk of the visit, and dictation fills in the gaps or adds precision where needed.
The Rise of Hybrid Workflows
If you look at what actually works in production environments, it’s rarely a single approach. The most effective systems combine multiple modes seamlessly. The best systems don’t force a single mode.
They combine:
- Ambient listening (capture everything)
- AI structuring (generate draft)
- Dictation (add precision)
- Manual edits (final control)
A typical workflow today looks something like this:
During the consultation, ambient listening runs quietly in the background. The clinician doesn’t have to think about documentation at all.
After the visit, they review the generated note. Maybe they tweak a few lines, maybe they dictate an additional observation, maybe they restructure a section.
Then they finalize.
This hybrid model works because it balances automation with control. Ambient AI ensures nothing is missed, while dictation and manual edits ensure accuracy and clinical intent.
Trying to replace one with the other doesn’t work as well. Combining them does.
What’s Getting Better
Voice is no longer just about documentation it’s becoming a clinical intelligence layer.
Beyond the core workflows, there are a few areas where voice-enabled documentation is rapidly improving.
One is specialty awareness. Systems are getting better at understanding context—what matters in a cardiology note is different from behavioral health or primary care. Templates and summaries are becoming more tailored, which reduces the need for heavy editing.
Another is clinical intelligence. Modern tools don’t just document—they start to assist. They can identify potential diagnoses, suggest codes, or highlight missing information. In some cases, they even prompt clinicians in real time if something important hasn’t been addressed.
Multilingual capabilities are also improving. Real-time transcription and translation are making it easier to handle diverse patient populations without breaking workflow.
And then there’s voice as a control layer. Not just dictating notes, but navigating the EHR itself adding sections, inserting data, triggering actions—without touching the keyboard.
Where Things Still Fall Short
For all the progress, it’s not perfect.
Accuracy can still drop in noisy environments or when multiple people speak at once. Accents and speech patterns can introduce variability. And while AI is good at summarizing, it doesn’t always capture nuance the way a clinician would.
There’s also the issue of trust. Clinicians need to feel confident that what’s being documented is correct. That’s why review and edit steps are still essential.
And finally, integration matters more than anything. Even the best voice technology fails if it doesn’t fit cleanly into the EHR workflow. If it adds friction instead of removing it, adoption drops quickly.
What This Means for EHR Design
If you’re building or evaluating voice capabilities in an EHR, the takeaway is clear: this isn’t just a feature it’s a workflow layer.
The systems that work today share a few common principles:
- They stay out of the way during the visit.
- They support multiple input modes, not just one.
- They generate structured, usable output not just text.
- They always keep the clinician in control of the final note.
- And they maintain a clear audit trail of what was captured, generated, and edited.
How Elixir Approaches Voice Differently
In Elixir, voice is not a plugin. It’s embedded into the core clinical workflow through the AI Co-Pilot.
Ambient-First Design
- Works across physical and virtual visits
- Zero disruption to provider workflow
Structured Intelligence
- Automatic mapping to clinical templates
- Context-aware note generation
Multi-Modal Flexibility
- Ambient + Dictation + Manual editing
- Clinician always in control
End-to-End Traceability
- Audio → Transcript → AI Output → Final Note
- Fully auditable for compliance
The Bottom Line
Voice recognition in healthcare has finally moved beyond being a productivity tool. It’s becoming foundational to how clinical documentation happens.
But the winners aren’t the systems that simply “convert speech to text.”
They’re the ones that can listen, understand, structure, and assist without getting in the way.
We’re not just moving toward voice-enabled EHRs.
We’re moving toward documentation that happens naturally, as care happens.
Recent Posts
Common Pitfalls in Healthcare Billing and How to avoid them
Categories
Archives
- May 2026
- April 2026
- March 2026
- December 2025
- November 2025
- September 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- November 2024
- September 2024
- July 2024
- April 2024
- February 2024
- November 2023
- September 2023
- August 2023
- May 2023
- February 2023
- January 2023
- July 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- March 2021
- October 2020
- May 2020


Recent Comments