Healthcare Cybersecurity Protecting Your EHR in 2026

Introduction
Here is something no vendor brochure will say plainly: most healthcare organizations in 2026 are still one phishing email away from a serious breach. The tools have improved. The attackers have improved faster.
Electronic Health Records hold a patient’s most sensitive information — diagnoses, medications, mental health notes, financial data. Protecting that data is not just a legal requirement. It is a fundamental duty to the people who trust you with it.
This guide cuts through the noise. We will cover the real threats, where EHR security breaks down, what HIPAA demands in 2026, and the practical steps you can take starting this quarter.
A patient’s medical record is worth up to 40 times more than a stolen credit card on the dark web. Cybercriminals know this. Does your security posture reflect it?
Why Healthcare Is Always the Top Target
Healthcare has led to breach statistics for 14 consecutive years. In 2025, over 700 reported breaches were exposed to more than 180 million patients. This is not coincidence it is structure.
The core reasons attackers keep coming back:
- Medical devices run outdated software that cannot be safely patched — creating permanent, known vulnerabilities on clinical networks.
- Clinical staff prioritize speed of care over security steps, creating enormous pressure to cut corners on authentication.
- EHR systems are deeply integrated with dozens of third-party vendors — every connection is a potential entry point.
- Ransomware attacks hit harder in healthcare because patient care cannot wait. Criminals know hospitals are more likely to pay.
- Health records cannot be “cancelled” like a credit card — they hold lifelong data that enables insurance fraud, identity theft, and blackmail.
Key Principle
HIPAA compliance is the legal minimum — not a security strategy. Organizations that treat it as a finish line are still exposed.
The 2026 Threat Landscape
AI-Powered Phishing
The old advice check for spelling mistakes no longer applies. Attackers now use AI to craft emails that reference real colleagues, real systems, and real institutional language. A clinician receives a message appearing to come from IT about an EHR update and clicks a login link. Credentials were stolen. It is that simple now.
Double & Triple Extortion Ransomware
Modern ransomware groups do not just lock your systems they first steal your data. Then they threaten to publish sensitive patient records publicly if you do not pay. Some groups even contact patients directly. The result: one attack triggers a business continuity crisis, a HIPAA violation, and a reputational disaster simultaneously.
Supply Chain Attacks
The 2024 Change Healthcare attack affected over 100 million patients and the target was not a hospital. It was a billing clearinghouse. Your security is only as strong as your weakest vendor connection. Every third-party integration into your EHR is a potential door for attackers to walk through.
Insider Threats
A significant share of healthcare breaches involves people inside the organization staff accessing records out of curiosity, employees emailing PHI to personal accounts “for convenience, or former employees whose credentials were never deactivated. This is not always malicious. But the damage is the same.
REAL Example
A regional hospital in 2025 discovered a telehealth vendor had been exposing patient records through an unsecured API for over four months. The vendor had a signed BAA and was “HIPAA compliant.” The integration had never been independently security-tested after go-live.
The Numbers That Matter
$10.9M
Average cost of a healthcare breach in 2025 – highest of any industry
277 Days
Average time to detect and contain a healthcare breach
74%
Breaches involving a human element — phishing, stolen credentials, misuse
1 in 3
Ransomware victims in healthcare that paid the ransom in 2025
Where EHR Security Breaks Down
Access Rights Set Once, Never Revisited
Staff change roles. Contractors finish projects. Employees leave. But their access levels stay exactly where they were set sometimes for years. This is one of the most common and dangerous gaps in healthcare EHR security. Quarterly access audits and automated offboarding (disabling accounts within 24 hours of departure) are non-negotiable.
Audit Logs Nobody Reads
Every EHR generates detailed access logs. Most organizations collect them into a monitoring system that nobody actively reviews until after a breach. Automated alerting for anomalous behavior (bulk record downloads, off-hours logins, access outside a user’s normal specialty) turns passive data collection into active defense.
Encryption Gaps in Transit
Your data is encrypted at rest that is standard. But is it encrypted in transit between your EHR and your lab system, your patient portal, your cloud backup? Expired TLS certificates, misconfigured API connections, and unencrypted data flows are common vulnerabilities that often go undetected until it is too late.
Third-Party Integrations Left Unreviewed
That integration you set up with a telehealth vendor two years ago when did you last review its security posture? API connections into your EHR need regular security assessments, not just a one-time setup review. The threat landscape changes: your vendor oversight needs to keep pace.
Plain-Language Summary
Think of your EHR as a hospital building. Access rights are keys. Audit logs are security cameras. Encryption is the safe inside. Third-party integrations are side doors. Most organizations have good locks on the front door but several side doors are propped open.
HIPAA in 2026: What Has Actually Changed
HIPAA’s core requirements have not changed dramatically but enforcement has. The HHS Office for Civil Rights has sharply increased settlement amounts and is now actively scrutinizing whether organizations are practicing security, not just documenting it.
Cybersecurity Performance Goals (CPGs)
HHS released voluntary Cybersecurity Performance Goals for healthcare in 2023. While technically optional, organizations that cannot demonstrate CPG alignment face significantly harder regulatory conversations after a breach. Key areas: multi-factor authentication, email security, patching cadence, and incident response planning.
Business Associate Oversight
A signed BAA is no longer enough. Regulators now expect covered entities to conduct ongoing due diligence on vendors who handle PHI — not just collect a signed agreement and move on. High-risk vendors should face annual security reviews and provide written attestations.
Patient Right of Access
OCR continues to aggressively enforce the 30-day rule for patient records access requests. Many violations stem from EHR configuration issues or slow internal processes — not bad intent. But fines are equally real regardless of the cause. Review your access request workflows now.
HIPAA Quick Reference
The Security Rule requires three safeguard categories: (1) Administrative policies, training, risk assessments; (2) Physical device security, facility controls, workstation management (3) Technical access controls, audit logs, encryption, automatic logoff. All three are required — not optional, not aspirational.
Your Practical Action Plan
Do These First — High Impact Achievable Now
- Enable phishing-resistant MFA for all EHR logins. FIDO2 or passkey-based authentication is the 2026 gold standard. This single step prevents most credential-based attacks.
- Audit all user accounts. Disable inactive accounts (no login in 60+ days). Confirm all departed employees’ credentials are deactivated. Fix access levels that no longer match current roles.
- Document your incident response plan and test it. Run a tabletop exercise with clinical and executive leadership before a breach forces the conversation.
- Set up automated alerting on EHR audit logs bulk access, off-hours logins, geographic anomalies. If you lack internal capacity, a managed security provider is a strong option here.
Plan for This Quarter
- Commission a penetration test specifically targeting your EHR and its third-party integrations integrations, not just your general network.
- Review and update all Business Associate Agreements. Include specific security requirements, not just generic HIPAA language. Require annual security attestations from high-risk vendors.
- Implement network segmentation to isolate clinical systems and medical devices from administrative and guest networks.
- Deliver role-specific security training. Nurses, billing staff, and administrators face different threats — their training should reflect that.
Build Into Ongoing Operations
- Quarterly access rights review scheduled, assigned, documented.
- Annual HIPAA risk assessment with a real remediation roadmap, not a filed report.
- Regular backup testing knowing backups exist is not the same as knowing they work.
- Board-level cybersecurity reporting ties security posture to patient safety outcomes.
Security Is a Patient Safety Issue
When a ransomware attack forces a hospital to divert ambulances, delay surgeries, or take imaging systems offline that is not a technology problem. That is a patient safety crisis. When a rural hospital shuts down entirely after a catastrophic breach, the community loses its only emergency facility within 40 miles. These are documented realities, not hypotheticals.
Patients share information with their healthcare providers that they share with no one else on earth. They do this out of necessity and trust Protecting that information is what makes healthcare healthcare.
The organizations doing this well in 2026 have one thing in common: security is treated as a leadership responsibility, not an IT problem. Start there. Ask the right questions — when did we last test our incident response plan? Which vendors have access to our patient data? What happens if our EHR is offline for 72 hours? The technical controls follow once the culture and accountability are in place. And the patients your organization serves deserve nothing less.
About This Article
Written for healthcare practitioners, compliance officers, and clinical leaders. Statistics are drawn from IBM’s 2025 Cost of a Data Breach Report, HHS OCR enforcement records, and the HHS Healthcare Cybersecurity Performance Goals. This article reflects the author’s independent practitioner perspective and does not constitute legal or compliance advice.
Recent Posts
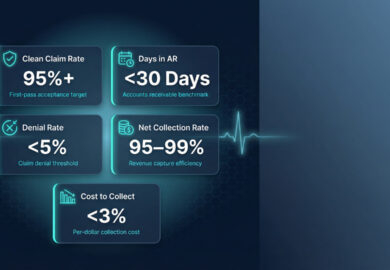
5 EHR Metrics to Improve Revenue Cycle & Healthcare IT
Categories
Archives
- April 2026
- March 2026
- December 2025
- November 2025
- September 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- November 2024
- September 2024
- July 2024
- April 2024
- February 2024
- November 2023
- September 2023
- August 2023
- May 2023
- February 2023
- January 2023
- July 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- March 2021
- October 2020
- May 2020

Recent Comments